- Gleneagles Medical Centre 6 Napier Road, #09-19, Singapore 258499
We strive to help you manage urogynaecologic symptoms so you can get back to living your best life. Book consultation with Dr Arthur Tseng now!
Pelvic organ prolapse (POP) is the symptomatic descent of one or more of the following:
- the anterior vaginal wall and the bladder (cystourethrocele),
- the posterior vaginal wall with the rectum (rectocele), and
- the apex (cervix/uterus) or vault (cuff after hysterectomy) of the vagina, resulting in utero-vaginal and vault prolapse respectively.
Medical care has improved, but many people often ignore pelvic organ prolapse (POP) and it worsens their lives. POP can become increasingly more prevalent as our population continues to age, especially among baby boomers. As chronic diseases become more manageable, we need to focus on POP and provide attention and care. This is important to ensure a good quality of life for our aging population.
Pelvic organ prolapse occurs in different types, depending on which pelvic organ is affected. These types include:
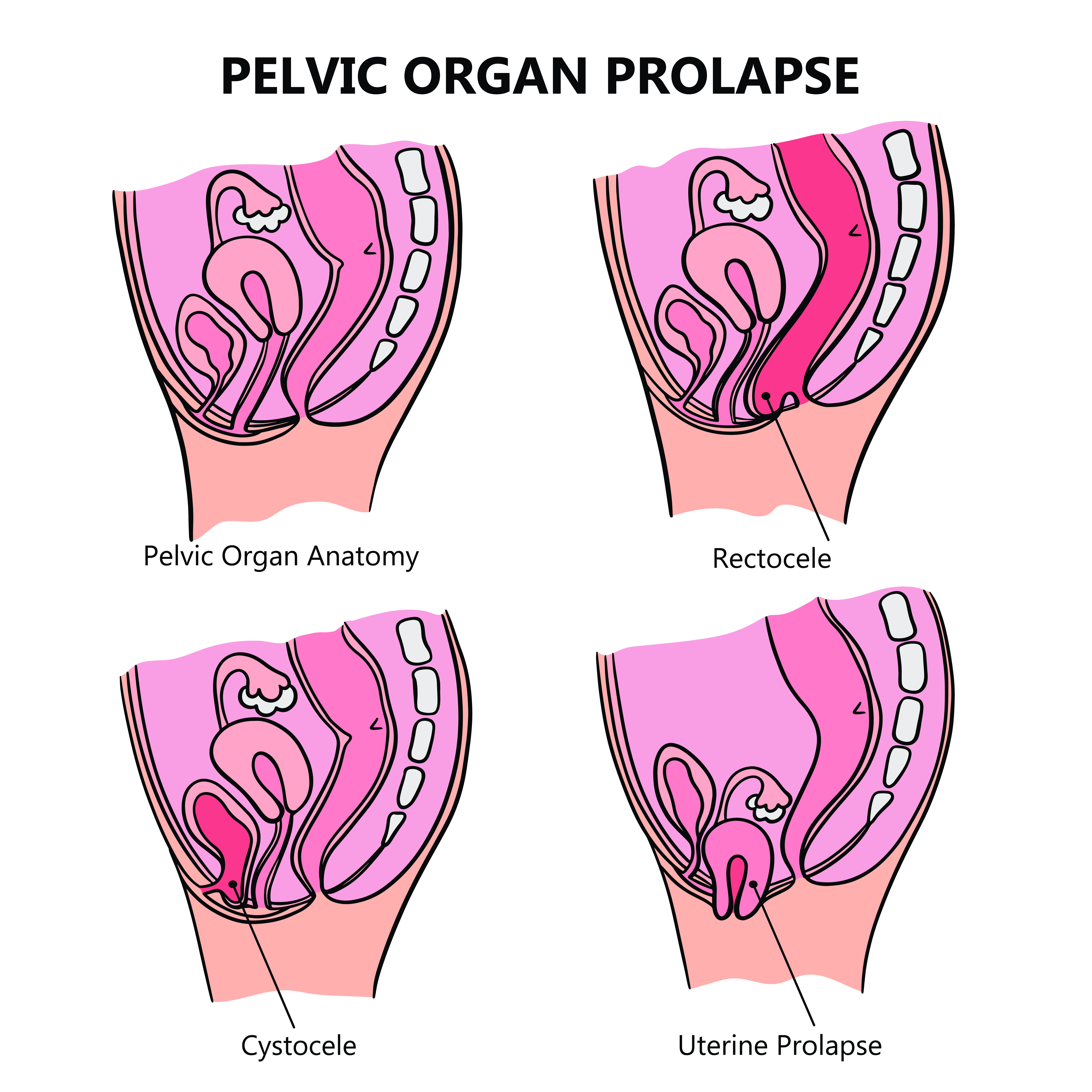
The organs in the pelvis are held up by muscles, tissue, ligaments, and nerves called the pelvic floor. When these formations weaken or stretch, the organs can move from their normal place, causing pelvic organ prolapse. Factors that increase the risk of POP encompass:
Some women with pelvic organ prolapse may not have any symptoms, while others may experience the following:
Dr Arthur Tseng has a lot of experience caring for women with pelvic floor problems and POP. He uses his knowledge to manage POP by creating personalized treatment plans for each patient.
The goal of treatment is to relieve symptoms and restore pelvic organ support. You can use non-surgical treatments such as lifestyle changes, physical therapy, or a pessary to manage POP.
Patients who can’t or don’t want surgery can use a vaginal pessary. You can also use it temporarily while waiting for surgery. The most commonly used type of pessary is the ring pessary, designed to both support and alleviate prolapse symptoms.
People who use a pessary should undergo pelvic exams every 3-4 months. However, this is not necessary if they are able to insert and remove the pessary on their own.
Surgical intervention in the vagina is the preferred remedial procedure for individuals suffering from Pelvic Organ Prolapse (POP). The surgery will involve cutting the vagina and fixing the muscles, ligaments, and tissue that hold up the organs. Doctors use different techniques to put organs back in place, depending on the type of prolapse.
Some procedures for treating certain conditions in women include vaginal hysterectomy, Manchester’s operation, colporrhaphy, pelvic floor repair, and sacrospinous ligament fixation. This last procedure involves attaching the top of the vagina to a ligament using non-absorbable sutures.
In some cases, doctors may also place a mesh/graft between layers of tissue or muscle to help support and strengthen the pelvic floor.
After surgery, you may need to use a pessary for added support while your body recovers. Your surgeon may also suggest lifestyle changes such as weight loss and exercise to improve your recovery process.
You can’t control some risk factors for pelvic organ prolapse, such as getting older and being pregnant. But there are things you can do to lower your chances of getting this condition, such as:
If you have symptoms of pelvic organ prolapse, Dr. Arthur Tseng can evaluate and treat you. He dedicates himself to helping his patients manage their condition and achieve the best possible outcome!
Dr Tseng's expertise covers urinary incontinence and pelvic organ prolapse, apart from that, his particular interest lies in the holistic management of Overactive Bladder Syndrome and other functional bladder conditions. With many years of experience in this field, he is committed to providing patients